Colostomy surgery

We learn the ins and outs of the colostomy surgery procedure.
What is a colostomy?
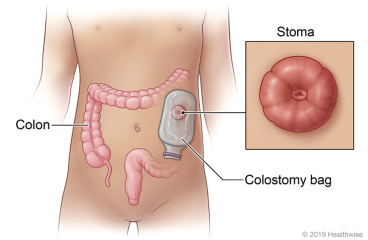
A colostomy is an operation that creates an opening for the large bowel to exit through the abdominal wall. The end of the large bowel is stitched to the skin to form an opening, called a stoma.
Why do I need a colostomy?
A colostomy may be needed if, as the result of an illness, injury or problem with your digestive system, or you can’t pass stools through your anus.
You may have a colostomy to treat:
- Colon/rectal cancer
- Crohn’s disease
- Diverticulitis
- Anal cancer
- Vaginal or cervical cancer
- Bowel incontinence
A colostomy is often used after a section of the colon has been removed and the bowel can’t be joined back together. This may be temporary and followed by another operation to reverse the colostomy later, or it may be permanent.
The colostomy surgery usually takes place at the same time of the removal of the tumour. Though, this depends on the type of cancer you have.
What happens before the procedure?
You would need to stop blood thinning medications and avoid food and drink for four hours before surgery. Regular medications are usually taken on the day. There is usually no need for bowel preparation/cleansing.
The most important part of colostomy surgery is meeting a stomal therapist, who is a specially trained nurse that deals with all aspects of stoma care. He/she will visit and discuss the details of living with a colostomy. Together an ideal spot on the tummy will be chosen and marked. This is important to ensure a comfortable and safe colostomy.
How is the procedure performed?
A colostomy is carried out under general anaesthetic, using either:
- Open surgery (laparotomy) – where a long cut (incision) is made in the tummy to access the colon.
- Laparoscopic (keyhole surgery) – where the surgeon makes several smaller incisions and uses a tiny camera and surgical instruments to access the colon.
Generally, keyhole surgery is the preferred option because recovery is quicker and the risk of complications are lower.
There are two main types of colostomy: a loop colostomy and an end colostomy. The specific technique used will depend on your circumstances.
What are the risks?
The laparoscopic port sites may develop wound sepsis, a haematoma (blood clot) in the wound or a seroma (drainage of clear fluid). The stoma itself rarely develops wound infections.
After surgery, narrowing of the colostomy, skin irritation or small amounts of bleeding from the stoma may occur. Late complications (weeks/months) include scar tissue causing bowel blockages and a hernia developing at the stoma site.
There are medications to manage these side effects. It is always important to report any side effects to your stomal therapist.
What happens after the procedure?
You may be able to suck on ice chips on the same day as your surgery. You’ll probably be eating by the next day. Most people would be able to head home in three to five days.
A normal stoma is moist and pink or red coloured. When you first see your colostomy, it may appear dark red and swollen, with bruises. Don’t worry. Within a few weeks, the colour will lighten and bruises should disappear.
How will I manage with my new stoma?
While you recover in hospital your stomal therapist will visit and show you how to care for your new stoma.
The number of sessions required before you are comfortable with stoma care varies from person to person. A family member may be present during these sessions to assist.
In general, your stoma is no hindrance to exercise, travel, working, socialising and intimacy. It’s important to give yourself time to get used to it. Thankfully, modern colostomy equipment is discreet and secure.
It’s extremely important to keep all appointments with your stomal therapist so you can get all the information and advice you need on how to care for it. Your stomal therapist can also introduce you to other stoma patients, as another way for you to have support on your road to recovery. It’s good to speak to someone who has been through the procedure.
Contributor - Dr Ebrahim Dalwai
Dr Ebrahim Dalwai is a subspecialist colorectal surgeon based at Life Kingsbury Hospital. He holds a senior lecturer position in the Colorectal Unit at Groote Schuur Hospital/University of Cape Town and is a partner in the Matley Practice.
Contributor - Anneké Bowley
Anneké Bowley is a stomal therapist working at Dee Waugh Stomaltherapy Services.